Pazopanib Selectively Inhibits Choroidal Vascular Endothelial Cell Proliferation and Promotes Apoptosis
Medical hypothesis discovery and innovation in ophthalmology,
Vol. 9 No. 1 (2020),
19 November 2019
,
Page 7-14
Abstract
Exudative age related macular degeneration (AMD) is related to active choroidal neovascularization (CNV) and formation of disciform scars. Vascular endothelial growth factor (VEGF) mediated choroidal vascular endothelial cell (CVECs) proliferation is characteristic of CNV. Intravitreal injections of bevacizumab, ranibizumab and aflibercept (anti-VEGF monoclonal antibodies) are used to treat exudative AMD. Pazopanib, a tyrosine kinase inhibitor, inhibits neovascularization through blockade of intracellular tyrosine kinase VEGF receptor and platelet-derived growth factor receptor. In this in vitro investigation, we evaluated the inhibitory consequences of escalating doses of pazopanib on proliferation of VEGF-enriched CVECs to establish a safe dosage range. VEGF (50 ng/mL) enriched CVECs were treated with escalating doses of pazopanib (10, 50,100 and 250 µM). Cell proliferation rates (WST-1 assay), cell viability (trypan blue exclusion assay), and reactive oxygen species (ROS) levels were measured at 48h, 72h and 1 week. Intracellular caspase 3 levels and morphological changes were recorded. VEGF enriched CVECs showed a significant decrease in cell proliferation rates after one week of treatment with increasing doses of pazopanib (10, 50,100 and 250 µM) treatment i.e. 87.8%, 43.0%, 38.1% and 9.3% compared to controls (p<0.001). Similarly, trypan blue exclusion assay revealed a decrease in cell viability as 81.8%, 81.0%, 53.4% and 8.7%, respectively (p<0.05). Further, pazopanib actively inhibited proliferation of VEGF-enriched CVECs, with 1.32, 1.92, 1.92 and 4.1-fold increase (p<0.01) in intracellular caspase 3 levels. VEGF-enriched CVECs treated with escalating doses of pazopanib decreased cell viability and increased caspase 3 levels in a time and dose dependent manner.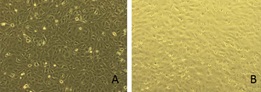
References
Gehrs KM, Anderson DH, Johnson LV, Hageman GS. Age-related macular degeneration--emerging pathogenetic and therapeutic concepts. Ann Med. 2006;38(7):450-71. doi: 10.1080/07853890600946724 pmid: 17101537
Congdon N, O'Colmain B, Klaver CC, Klein R, Munoz B, Friedman DS, et al. Causes and prevalence of visual impairment among adults in the United States. Arch Ophthalmol. 2004;122(4):477-85. doi: 10.1001/archopht.122.4.477 pmid: 15078664
Chalam KV, Balaiya S, Malyappa RS, Hsi W, Brar VS, Murthy RK. Evaluation of choroidal endothelial cell proliferation after exposure to varying doses of proton beam radiation. Retina. 2011;31(1):169-76. doi: 10.1097/IAE.0b013e3181dee621 pmid: 20829738
Photodynamic therapy of subfoveal choroidal neovascularization in age-related macular degeneration with verteporfin: one-year results of 2 randomized clinical trials--TAP report. Treatment of age-related macular degeneration with photodynamic therapy (TAP) Study Group. Arch Ophthalmol. 1999;117(10):1329-45. pmid: 10532441
Isola V, Pece A, Pierro L. Photodynamic Therapy With Verteporfin of Choroidal Malignancy From Breast Cancer. American Journal of Ophthalmology. 2006;142(5):885-7. doi: 10.1016/j.ajo.2006.06.008
Mynampati BK, Sambhav K, Grover S, Chalam KV. Inhibition of proliferation of retinal vascular endothelial cells more effectively than choroidal vascular endothelial cell proliferation by bevacizumab. Int J Ophthalmol. 2017;10(1):15-22. doi: 10.18240/ijo.2017.01.03 pmid: 28149771
Bhutto I, Lutty G. Understanding age-related macular degeneration (AMD): relationships between the photoreceptor/retinal pigment epithelium/Bruch's membrane/choriocapillaris complex. Mol Aspects Med. 2012;33(4):295-317. doi: 10.1016/j.mam.2012.04.005 pmid: 22542780
Mohan N, Monickaraj F, Balasubramanyam M, Rema M, Mohan V. Imbalanced levels of angiogenic and angiostatic factors in vitreous, plasma and postmortem retinal tissue of patients with proliferative diabetic retinopathy. J Diabetes Complications. 2012;26(5):435-41. doi: 10.1016/j.jdiacomp.2012.05.005 pmid: 22699109
Kim SY, Mocanu C, McLeod DS, Bhutto IA, Merges C, Eid M, et al. Expression of pigment epithelium-derived factor (PEDF) and vascular endothelial growth factor (VEGF) in sickle cell retina and choroid. Experimental Eye Research. 2003;77(4):433-45. doi: 10.1016/s0014-4835(03)00174-x
Vasudev NS, Reynolds AR. Anti-angiogenic therapy for cancer: current progress, unresolved questions and future directions. Angiogenesis. 2014;17(3):471-94. doi: 10.1007/s10456-014-9420-y pmid: 24482243
Zhou J, Shukla VV, John D, Chen C. Human Milk Feeding as a Protective Factor for Retinopathy of Prematurity: A Meta-analysis. Pediatrics. 2015;136(6):e1576-86. doi: 10.1542/peds.2015-2372 pmid: 26574589
Yang S, Zhao J, Sun X. Resistance to anti-VEGF therapy in neovascular age-related macular degeneration: a comprehensive review. Drug Des Devel Ther. 2016;10:1857-67. doi: 10.2147/DDDT.S97653 pmid: 27330279
Boyer DS, Hopkins JJ, Sorof J, Ehrlich JS. Anti-vascular endothelial growth factor therapy for diabetic macular edema. Ther Adv Endocrinol Metab. 2013;4(6):151-69. doi: 10.1177/2042018813512360 pmid: 24324855
Al-Khersan H, Hussain RM, Ciulla TA, Dugel PU. Innovative therapies for neovascular age-related macular degeneration. Expert Opin Pharmacother. 2019;20(15):1879-91. doi: 10.1080/14656566.2019.1636031 pmid: 31298960
Barakat MR, Kaiser PK. VEGF inhibitors for the treatment of neovascular age-related macular degeneration. Expert Opin Investig Drugs. 2009;18(5):637-46. doi: 10.1517/13543780902855316 pmid: 19388880
Chappelow AV, Kaiser PK. Neovascular age-related macular degeneration: potential therapies. Drugs. 2008;68(8):1029-36. doi: 10.2165/00003495-200868080-00002 pmid: 18484796
Mousa SA, Mousa SS. Current status of vascular endothelial growth factor inhibition in age-related macular degeneration. BioDrugs. 2010;24(3):183-94. doi: 10.2165/11318550-000000000-00000 pmid: 20210371
Ni Z, Hui P. Emerging pharmacologic therapies for wet age-related macular degeneration. Ophthalmologica. 2009;223(6):401-10. doi: 10.1159/000228926 pmid: 19622904
Danis R, McLaughlin MM, Tolentino M, Staurenghi G, Ye L, Xu CF, et al. Pazopanib eye drops: a randomised trial in neovascular age-related macular degeneration. Br J Ophthalmol. 2014;98(2):172-8. doi: 10.1136/bjophthalmol-2013-303117 pmid: 24227801
Suda K, Murakami T, Gotoh N, Fukuda R, Hashida Y, Hashida M, et al. High-density lipoprotein mutant eye drops for the treatment of posterior eye diseases. J Control Release. 2017;266:301-9. doi: 10.1016/j.jconrel.2017.09.036 pmid: 28987881
Ozkaya A, Alkin Z, Yazici AT, Demirok A. Comparison of intravitreal ranibizumab in phakic and pseudophakic neovascular age-related macular degeneration patients with good baseline visual acuity. Retina. 2014;34(5):853-9. doi: 10.1097/IAE.0000000000000024 pmid: 24141904
McLaughlin MM, Paglione MG, Slakter J, Tolentino M, Ye L, Xu CF, et al. Initial exploration of oral pazopanib in healthy participants and patients with age-related macular degeneration. JAMA Ophthalmol. 2013;131(12):1595-601. doi: 10.1001/jamaophthalmol.2013.5002 pmid: 24113783
Csaky KG, Dugel PU, Pierce AJ, Fries MA, Kelly DS, Danis RP, et al. Clinical evaluation of pazopanib eye drops versus ranibizumab intravitreal injections in subjects with neovascular age-related macular degeneration. Ophthalmology. 2015;122(3):579-88. doi: 10.1016/j.ophtha.2014.09.036 pmid: 25432081
Takahashi K, Saishin Y, Saishin Y, King AG, Levin R, Campochiaro PA. Suppression and regression of choroidal neovascularization by the multitargeted kinase inhibitor pazopanib. Arch Ophthalmol. 2009;127(4):494-9. doi: 10.1001/archophthalmol.2009.27 pmid: 19365030
- Abstract Viewed: 877 times
- Free Full Text PDF Downloaded: 535 times


