Preliminary Outcomes of Temporary Collagen Punctal Plugs for Patients with Dry Eye and Glaucoma
Medical hypothesis discovery and innovation in ophthalmology,
Vol. 9 No. 1 (2020),
19 November 2019
,
Page 56-60
Abstract
The aim of this study was using a temporary collagen punctal plug as a pre-test before decision of permanent punctal closure or long-term plug use for patients with dry eye disease (DED) and primary open-angle glaucoma (POAG). This case-control study was conducted at a single office in Honolulu, Hawaii from January 2017 to August 2018. In the case group, a temporary collagen plug was used in 33 eyes of 33 patients with DED and POAG who were receiving glaucoma medications with good control. On the other hand in the control group, 33 eyes of 33 patients with DED and POAG who were receiving glaucoma medications with good control were included, but punctal plug was not used. In the case group, one of the lower lid puncta was selected for the study and a canalicular rod shape plug was inserted as a therapeutic trial to predict the efficacy of long-term punctal plug placement or punctal closure. The mean changes of intraocular pressure (IOP) and improvement in symptoms/signs of DED were compared between the two study groups. Results revealed a statistically significant IOP reduction in the case group compared to the control group. Furthermore, DED improved significantly more in the case group compared to the control group (P< 0.001). We concluded that temporary punctal plug in patients with DED and POAG can significantly improve DED and lower IOP. Therefore, we could consider permanent punctal closure or long-term plug for patients with DED and POAG who responded well to temporary punctal plug without epiphora or other complications.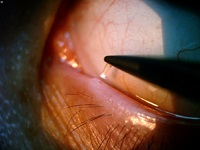
References
Moss SE, Klein R, Klein BE. Prevalence of and risk factors for dry eye syndrome. Arch Ophthalmol. 2000;118(9):1264-8. doi: 10.1001/archopht.118.9.1264 pmid: 10980773
Marcet MM, Shtein RM, Bradley EA, Deng SX, Meyer DR, Bilyk JR, et al. Safety and Efficacy of Lacrimal Drainage System Plugs for Dry Eye Syndrome: A Report by the American Academy of Ophthalmology. Ophthalmology. 2015; 122(8):1681-7. doi: 10.1016/j.ophtha.2015.04.034 pmid: 26038339
Song JS, Woo IH, Eom Y, Kim HM. Five Misconceptions Related to Punctal Plugs in Dry Eye Management. Cornea. 2018;37 Suppl 1:S58-S61. doi: 10.1097/ICO.0000000 000001734 pmid: 30211751
Mathews PM, Ramulu PY, Friedman DS, Utine CA, Akpek EK. Evaluation of ocular surface disease in patients with glaucoma. Ophthalmology. 2013;120(11):2241-8. doi: 10.1016/j.ophtha.2013.03.045 pmid: 23714318
Zimmerman TJ, Kooner KS, Kandarakis AS, Ziegler LP. Improving the therapeutic index of topically applied ocular drugs. Arch Ophthalmol. 1984;102(4):551-3. doi: 10. 1001/archopht.1984.01040030429017 pmid: 6704011
Huang TC, Lee DA. Punctal occlusion and topical medications for glaucoma. Am J Ophthalmol. 1989;107(2):151-5. doi: 10. 1016/0002-9394(89)90214-6 pmid: 2913809
Opitz DL, Tung S, Jang US, Park JJ. Silicone punctal plugs as an adjunctive therapy for open-angle glaucoma and ocular hypertension. Clin Exp Optom. 2011;94(5):438-42. doi: 10. 1111/j.1444-0938.2010.00587.x pmid: 21342261
Bartlett JD, Boan K, Corliss D, Gaddie IB. Efficacy of silicone punctal plugs as adjuncts to topical pharmacotherapy of glaucoma--a pilot study. Punctal Plugs in Glaucoma Study Group. J Am Optom Assoc. 1996;67(11):664-8. pmid: 8979659
Ervin AM, Law A, Pucker AD. Punctal occlusion for dry eye syndrome. Cochrane Database Syst Rev. 2017;6:CD006775. doi: 10.1002/14651858.CD006775.pub3 pmid: 28649802
Abby Gillogly O, Nicole Stout O, Nate Lighthizer O. Plug the Drain with Lacrimal Occlusion. Review of Optometry. 2016;June 15.
Tost FHW, Geerling G. Plugs for occlusion of the lacrimal drainage system. Dev Ophthalmol. 2008;41:193-212. doi: 10. 1159/000131090 pmid: 18453770
Craig JP, Nichols KK, Akpek EK, Caffery B, Dua HS, Joo CK, et al. TFOS DEWS II Definition and Classification Report. Ocul Surf. 2017;15(3):276-83. doi: 10.1016/j.jtos.2017.05.008 pmid: 28736335
Sherwin JC, Ratnarajan G, Elahi B, Bilkiewicz-Pawelec A, Salmon JF. Effect of a punctal plug on ocular surface disease in patients using topical prostaglandin analogues: a randomized controlled trial. Clin Exp Ophthalmol. 2018;46(8):888-94. doi: 10.1111/ceo.13311 pmid: 29700925
Raulin C, Greve B, Hartschuh W, Soegding K. Exudative granulomatous reaction to hyaluronic acid (Hylaform). Contact Dermatitis. 2000;43(3):178-9. pmid: 10985641
Ahn HB, Seo JW, Roh MS, Jeong WJ, Park WC, Rho SH. Canaliculitis with a papilloma-like mass caused by a temporary punctal plug. Ophthalmic Plast Reconstr Surg. 2009;25(5):413-4. doi: 10.1097/IOP.0b013e3181b57c01 pmid: 19966666
Mullins RJ, Richards C, Walker T. Allergic reactions to oral, surgical and topical bovine collagen. Anaphylactic risk for surgeons. Aust N Z J Ophthalmol. 1996;24(3):257-60. doi: 10.1111/j.1442-9071.1996.tb01589.x pmid: 8913129
Dana R, Bradley JL, Guerin A, Pivneva I, Evans AM, Stillman IO. Comorbidities and Prescribed Medications in Patients With or Without Dry Eye Disease: A Population-Based Study. Am J Ophthalmol. 2019;198:181-92. doi: 10.1016/j.ajo. 2018.10.001 pmid: 30312577
- Abstract Viewed: 991 times
- Free Full Text PDF Downloaded: 508 times


